
Part 1 was a call to action, an opportunity to reflect on your current practice. Part 2 will be a commitment to action. A commitment to say ‘I am haven’t mastered resuscitation, yet, but we’re going to get there.’ This may be a commitment to be the example while working in a status quo department. This may be the commitment to say that ‘I can’t choose how broken my system is, but I can choose to be the best provider regardless of those around me.’ This thinking isn’t an ego thing, but a realization and humbling to focus on what can be you as an individual can control. To fully embody this you must withhold judgement and focus on the only thing that’s within your control. You only control your thoughts and actions. Focus on the person looking in the mirror.

The Intubator’s Creed is adapted after the Rifleman’s Creed. There have been many versions adapted since WWII, but is better recognized within the Marine Corps.
The vision for the Intubator’s Creed is to recognize that we need to master the equipment and process of airway management, especially when teaching the next generations of providers. Heck, we should probably have paramedic students recite this before being released for their airway management clinicals.

Your laryngoscopes should be your best friends. Your best friends should be direct, video, and hyperangulated (HA). Some video laryngoscope (VL) systems are always HA regardless of the blade choice. Each one of them has a different technique on how to manipulate and utilize the device. Master the technique like you master your life.

A resuscitationist has multiple tools and techniques to manage the airway, a laryngoscope being one of them. A resuscitationist is a humble, confident provider who is able to know when to utilize the laryngoscope versus other tools. A resuscitationist knows when not to use a laryngoscope. They know that a laryngoscope and an ET tube is not the cure for their patients. They’re able to prevent the 3 deadly horsemen of intubation, hypoxia, hypotension, and aspiration, without using a laryngoscope. A resuscitationist is intentional about the manipulation of the laryngoscope. They’re able to use Progressive Laryngoscopy to get The View and know how each laryngoscope works. More to come in part 3.
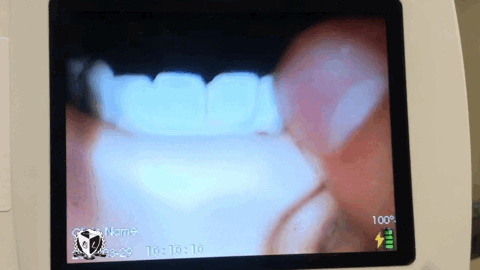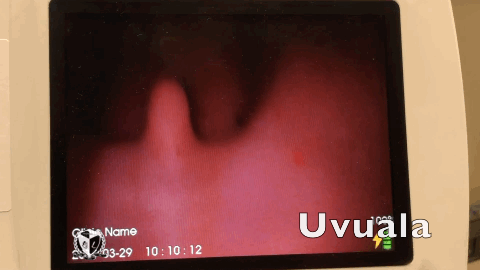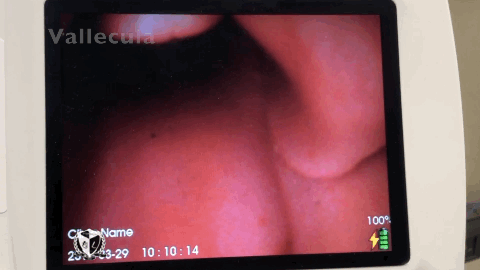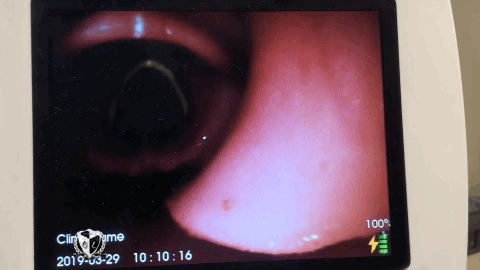

A laryngoscope in the hands of an inexpert can become a murder weapon. Be committed to learning your best friend. Don’t submit yourself to the laryngoscope, be the resuscitationist your patients deserve.

Providers are to serve their community, one patient at a time. We should strive for the Triple Aim to provide better care, improve the health of our community, at a lower cost. We can provide this service to our community when they’re the sickest by being steadfast in the aggressive care provided to send them home in a better state than when we met them. Even with mastering the laryngoscope there will still be airways which are not amenable to endotracheal intubation. There are going to be airways that a surgical airway is the first and only option. Providers don’t fail just because we don’t put plastic down their throat. Providers fail by not being intentional and extremely detailed in our approach to resuscitation and airway management. Providers fail by doing the same thing over and over again even in the face of evidence that they’re harming people. Providers fail when they don’t anticipate the difficult airway every single time. To serve people we have to become resuscitationist that are intentional, evidence based, and data driven.

Know how each one of them performs in all manners of environments. Test and decided, based on evidence, which one you’ll use for the various difficult airways presented by the HEAVEN Criteria. Find out when your laryngoscopes will let you down before you’re in a tough spot with an equipment failure. Have a plan to move on to the next step and practice with your laryngoscopes until you master them.
For heaven sakes make sure you have multiple options and proficiency with your laryngoscope. Don’t just always intubate with a 4 Mac Blade so ‘you’re prepared for all airways’! Using a Mac 4 for everyone takes up a large portion of the mouth and encourages intubators for to go too deep, which is the most common mistake when performing laryngoscopy. Being prepared for all airways is having an intentional plan with branch points that everyone understands.

Defend the airway with all tools available. Be intentional, methodical, and steadfast in your commitment to serve your patients through aggressive resuscitation and safe intubation.
-Adam LaChappelle (@vamedic on Twitter)
The master of disaster looking to practice good medicine in austere environments
