
The Laryngoscope:
The tool many wield, but only a resuscitationist masters

In the late 1800’s Alfred Kirstein developed the autoscope to directly visualize the glottis. Prior to this, mirrors were utilized to perform indirect laryngoscopy. Many of Alfred’s colleagues felt that there was not a need to directly view the glottis. Alfred stated “…Many a laryngoscopist is convinced that the laryngological technique needs no additions; others may think differently. Only the future can decide this question.”
The future decided to answer this question. Resuscitationist must be able to directly AND indirectly view the glottis depending on the laryngoscope utilized. The traditional direct laryngoscope blades, Mac and Miller, displace airway tissues by directly moving them anterior allowing the intubator the ability to place an endotracheal tube. The advent of video laryngoscope created dissension among intubators because the VL blades may not get a direct view of the glottis depending on if the VL blades are hyperangulated. Being hyperangulated means that this is another tool to aid in increasing FPS especially in the setting of difficult airway anatomy.
Know your equipment and where your eyes should be looking. Don’t try to get a direct view with a hyperangulated blade. Using a VL with a hyperangulated blade as a DL will result in suboptimal view and tube deliver.

A hyperangulated blade is meant to be non-displacing, meaning that the VL blade peaks around the corner of the tongue. The intubator must use the video screen to get an indirect view. This means that the intubator’s eyes should be on the screen instead of trying to get a direct view.

Examples of hyperangulated brands are King Vision, GlideScope, and UEScope. As well as the CMAC D-Blade. The use of a rigid stylet is required for optimal tube deliver with a hyperangulated blade. The use of a bougie with a hyperangulated blade will create frustration with tube delivery. Intubators will likely be able to place the bougie inside the glottis, but the geometry and flexibility of the bougie will often displace the tube posteriorly into the esophagus. The same is true with a flexible stylet in that once the tube meets resistance it will tend to bend the tube and stylet, failing to deliver the tube.

Deep dive into your equipment and try to break it. That’s right, find the limit of your equipment without running over it with your ambulance. This doesn’t mean being a meat head and trying to get a direct view with your VL when you have a perfectly good view on the screen. Becoming familiar with your equipment is knowing how each button works, how to change blades, how it operates in the bright light (outdoors and indoors). Get into the sim lab or grab a manikin and rigorously try different scenarios such as SALAD and Bloody Hell SALAD techniques. Use it before you loss it!
Intubating outdoors: Make sure if you’re using the VL outside that you try it out with everyone’s sunglasses on. Manufacturers use a polarized LCD screen to make it brighter. This means that if your polarized sunglasses are in the same orientation as the screen than the screen will appear black. Everyone’s sunglasses are different so make sure to check them out.

When practicing with the equipment you have it’s also important to perform a gradual step wised fashion of blade insertion utilizing progressive laryngoscopy. Be intentional about blade insertion. This allows the intubator to know where they’re at in the airway. Progressive laryngoscopy will prevent the intubator from placing the laryngoscope too deep in the airway or esophagus regardless if you’re using VL or DL. This will lead the intubator to get The View.

I’ve often heard providers state “I had a great view of the vocal cords, but I couldn’t the tube in!” This is because the blade is inserted too deep and directly displaced the epiglottis. This results in more of the laryngoscope taking up more of the peri-epiglottic space as well as an even more acute approach that the ET tube has to make to pass the vocal cords. To correct this the intubator should back the laryngoscope out and reinsert the laryngoscope into the vallecula.
The View is utilized to ensure that the blade is in the proper place to allow for enough room for tube delivery and not displacing the wrong airway tissue. The View consist of the laryngoscope blade in the vallecula allowing for a view of the epiglottis that is anterior to the glottis.

A high rolling resuscitationist will ensure that they’re intentional about getting The View every time utilizing progressive laryngoscopy.
Progressive laryngoscopy ensures that we know where we’re at in the airway and don’t jam the laryngoscope into the esophagus. Because right about that time someone will inevitably ask “What do you see?” which the reply is usually “I just see pink!” This common occurrence can be avoided by identifying 4 structures within the airway to get The View.
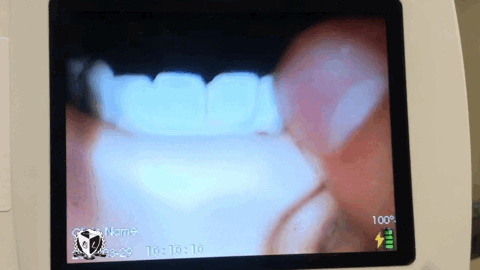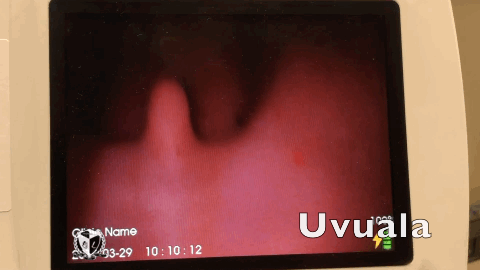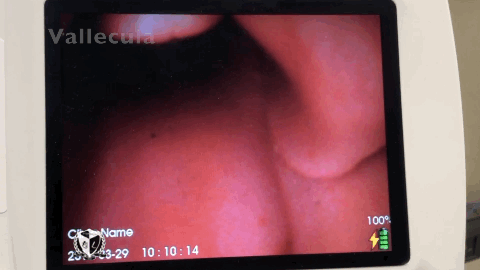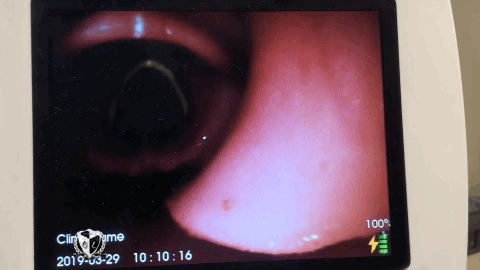
Laryngoscopy begins by inserting the laryngoscope midline instead of the traditional right sided approach. Using the right sided approach and performing a tongue sweep results in longer intubation time because it doesn’t create enough peri-epiglottic space to deliver the ET Tube. Approaching from the midline allows you to easily identify the first structure during progressive laryngoscopy, the uvula. The uvula is the directional sign of the airway, it points you to the epiglottis which is the second structure to find. Progressing to the epiglottis involves taking incremental steps to push the tongue out of the way. Finding the epiglottis prevents the intubator from placing the laryngoscope too deep. Take the laryngoscope and place it anterior to the epiglottis into the third structure, the vallecula. Seating the laryngoscope into the vallecula allows your to indirectly lift the epiglottis via the hyoepiglottic ligament.

Becoming a master resuscitationist requires that you are intentional; especially when approaching the airway. Know how to use your laryngoscope appropriately, break it through practice, and use progressive laryngoscope to get The View.
-Adam LaChappelle (@vamedic on Twitter)
The master of disaster looking to practice good medicine in austere environments
Reference:
Green-Hopkins, I., Werner, H., Monuteaux, M. C., & Nagler, J. (2015). Using Video-recorded Laryngoscopy to Evaluate Laryngoscopic Blade Approach and Adverse Events in Children. Academic Emergency Medicine: Official Journal of the Society for Academic Emergency Medicine, 22(11), 1283–1289. https://doi.org/10.1111/acem.12799
Jarvis, J. L., McClure, S. F., & Johns, D. (2015). EMS Intubation Improves with King Vision Video Laryngoscopy. Prehospital Emergency Care: Official Journal of the National Association of EMS Physicians and the National Association of State EMS Directors, 19(4), 482–489. https://doi.org/10.3109/10903127.2015.1005259
Nickson, C. (2019, March 22). Direct Laryngoscopy. Retrieved August 23, 2019, from Life in the Fast Lane • LITFL • Medical Blog website: https://litfl.com/direct-laryngoscopy/
Weingard, S. (2012, April 1). Airway Management with Rich Levitan. Retrieved August 23, 2019, from EmCrit Blog website: https://emcrit.org/emcrit/rich-levitan-airway-lecture/
